A new wonder drug, a princess and a missed opportunity to rid the world of its oldest disease
It is 40 years since the roll out of a new wonder drug to cure leprosy began to every corner of the globe. Since 1982, millions of people have avoided a lifetime of disability by taking Multidrug therapy (MDT).
MDT is a combination of three antibiotics, taken for six months to two years. After just two weeks, a person is no longer infectious. It was, and remains, the only effective cure for leprosy.
Back in 1982, the miracle trio of antibiotics brought with it a wealth of opportunity and a wave of optimism. But despite a real buzz of excitement in the Development sector, the roll out was slow. Leprosy is a disease of poverty affecting poor countries and, as a result, is low priority. The drug trials took a decade and it was 1995 before MDT reached every part of India. This in itself is shocking as India has always been home to more than half the world's leprosy cases.
By the 1990s, the number of people cured of leprosy globally each year climbed to around 750,000. Momentum was further fuelled by a World Health Organization goal of 'eliminating' leprosy by the Millennium. The elimination target was for less than one person in 10,000 to have leprosy.
Royal patronage and record numbers cured
It was an exciting time in the battle to defeat leprosy. The disease was getting regular mentions in the international news. The UK public even began to learn of the prejudice that goes hand in hand with the disease. This sparked the interest of the world's most photographed woman, Diana, Princess of Wales, who had a heart for the marginalised.
Borne out of her own feelings of loneliness and exclusion from the Royal family, Diana sought to reach out to people on the fringes of society. Whether it was visiting AIDS patients or shaking the hands of leprosy patients, Diana was not afraid of making a splash.

Diana soon became Patron of The Leprosy Mission. She made visits to Premananda Hospital in Kolkata, India, and Anandaban Hospital in Nepal, attracting press coverage around the globe. Even when she reduced her patronage of nearly 100 charities to just six in 1996, she continued her support of The Leprosy Mission. She remained an active Patron until her untimely death in 1997.
Diana's very public support and a worldwide effort to eliminate leprosy by 2000 saw record numbers cured in the 1990s. The global target was actually achieved, but unfortunately created a false sense of success. When the numbers fell below the one in 10,000 rate, governments redirected the money to treating other diseases.
MDT changes leprosy work in Nigeria
Jannine Ebenso, who supports leprosy research as part of her Senior Leadership role at The Leprosy Mission’s International office, began her career with The Leprosy Mission in 1991. She joined the charity as a physiotherapist and was seconded to Nigeria 30 years ago this month.
Jannine, who lives in Leeds, said: "MDT was a gamechanger and it was an exciting time joining the fight against leprosy in the 90s. MDT meant it was possible, for the first time, to completely cure leprosy. Previously, patients had to take the single antibiotic dapsone for their entire lifetime to manage the disease.

"I was in Nigeria for 16 years, first working with leprosy patients at the Qua Iboe Church Leprosy Hospital in the South-East of Nigeria. Our work saw us travel into the bush to help diagnose leprosy in remote communities and offer treatment with MDT. Our main goal was to give treatment as early as possible so as to prevent life-long disabilities.
"I learnt some of the local language, Efik, while living in the South-East but was relocated to the North-West of Nigeria in 1997. The area was found to have a huge number of undiagnosed leprosy cases. We put a few messages in churches, mosques, shops and other public places for people to come forward if they had any skin complaints. The first symptom of leprosy is often a light-coloured skin patch which is numb to the touch. Very quickly there was a queue stretching to right around the back of our clinic of people who wanted to be screened for leprosy.
"It was hard for the government health workers in the area to identify leprosy as they were looking after so many other diseases. They were also helping people with eye problems and delivering babies. It was easy for me to focus on leprosy as that was my job.
"I was now living in Hausa-Fulani land and so had to rely on my driver to translate a diagnosis, advice and health education to the patients. We had to relay the message somehow and amazingly always seemed to find a way!"
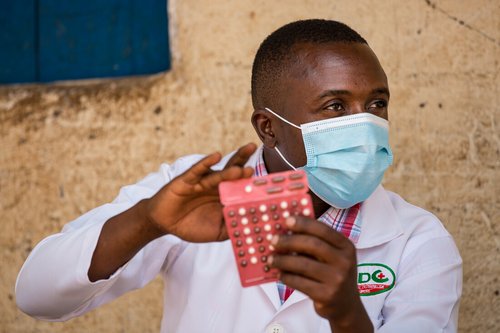
Photo: Ricardo Franco
The number of new leprosy cases diagnosed began to drop following the Millennium, reducing to around 250,000 cases a year in 2008. They have plateaued at this level ever since.
Jannine said: "Hitting the elimination target hindered the amazing progress that was being made in the fight against leprosy, because governments pulled out resources from leprosy programmes and put them elsewhere.
"The disease afflicts the remotest parts of some of the world’s poorest countries. Stigma surrounding leprosy also means that people are afraid to come forward for treatment.
"There are so many factors why the target gave a false sense of achievement. Devastatingly it created a sense that the threat of leprosy is disappearing. As a result, many health systems no longer deemed leprosy a priority and research money dried up."
The past, present and future of MDT
Leprosy is one of the World Health Organization’s 20 Neglected Tropical Diseases, diseases that should not exist in the 21st century.
There is evidence to suggest that in 2020 there were four million people living with untreated leprosy. This means for every person cured of leprosy today, there are 19 ‘hidden’ cases that need to be found and treated. Prejudice, lack of knowledge and insufficient healthcare sees leprosy continue to affect entire communities. These are largely poor communities. Overcrowding, malnutrition and a lack of sanitation are factors that lead to weakened immune systems, meaning people are more likely to catch the disease.
Dr Premal Das (pictured below) is a reconstructive surgeon and heads up The Leprosy Mission’s work in India. He has restored mobility to disabled hands and feet for more than 30 years. Dr Premal’s family has a great legacy: his grandfather was a Leprosy Mission doctor in the 1890s and was visited by Wellesley Bailey, the founder of The Leprosy Mission, himself. His father, uncle, aunts, and cousins also served the Mission as doctors and surgeons. Dr Premal married his wife, Dr Loretta Das, after the couple met at Christian Medical College in Vellore. They joined The Leprosy Mission in 1985.

Dr Premal said, as a young child in the 1960s, he remembered seeing children coming to the hospital.
"The whole family would be crying," he recalled.
"Back then if you had leprosy that was it; you had to stay at the hospital for the rest of your life. The patients were well cared for and were allowed to see visitors outdoors. But, as you can imagine, this did little to numb the pain of leaving your child at a hospital forever.
"I knew MDT was on its way when I was a medical student in Vellore. My first few years at The Leprosy Mission were spent in the community, finding, and curing leprosy with the new wonder drug.
"We would carry large jars of water and set up a village clinic under a tree. MDT was an expensive medicine and there was a vibrant black market. It had to be given as a supervised dose. We had to make sure the medicine had been swallowed by pouring water down patients’ throats.
"It would be a nightmare if we didn’t have MDT. In my lifetime alone so much has changed because of this treatment.
"The challenge now is that we need more new drugs and treatments. We need to be prepared for drug resistance to MDT. Treating leprosy in its early stages is vital to prevent disability. Better diagnostic tools are the way forward. Catching the disease early is essential to stop the spread. It is paramount to ending leprosy.”